Science report
A round-up of the latest science stories in Cambridge University as part of our new weekly strand.
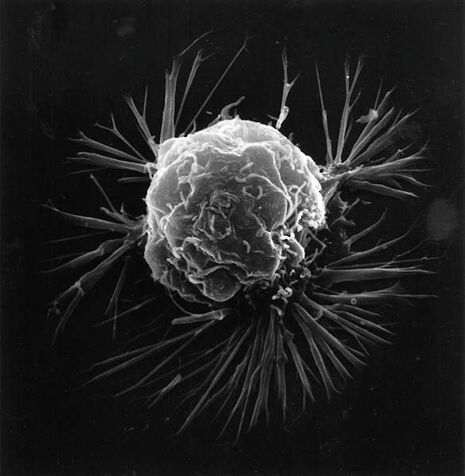
Researchers at the University have found that hundreds of lives could be prolonged through more effective breast cancer diagnosis in poorer areas.
Survival rates would be greater if hundreds of women living in England’s more deprived areas had diagnosis at the same stage as those in more affluent areas.
Working with scientists at the University of Leicester, researchers at the University of Cambridge looked at how much of a difference late-stage diagnosis had on women from deprived areas.
Dr Mark Rutherford, of the Department of Health Sciences at the University of Leicester, said: “We found that for a typical yearly cohort of breast cancer patients in England, 450 deaths could have been postponed beyond 5 years of diagnosis if the stage distribution for all women matched that of the most affluent.”
A means of reducing the inequality in the diagnosis of breast cancer is significant in the reduction of inequalities in breast cancer survival, even in the short-term. Dr Martine Bomb, head of early diagnosis at Cancer Research UK, said: “More needs to be done to tackle this inequality to ensure everyone has the same chance of surviving breast cancer, no matter where they live.”
Funding for the research was provided by both Cancer Research UK and The National Institute for Health Research (NIHR). Their work will be published in the International Journal of Cancer.
---------------------------

A team of scientists from the University of Cambridge have identified so-called ‘pest’ species – the ‘dirty dozen’ – that could wipe out native species and cause millions of pounds worth of damage clogging up drains by growing in large colonies in Britain’s water ways.
Among the several species is the ‘clogger mussel’, purported to be the worst threat to the UK. Though they are only the size of a thumb nail, clusters of the quagga mussels, their official name, can grow to a thickness of several metres.
This species of mussel is expected to arrive in the country in the next five years. Dr Belinda Gallardo outlined the damage to not only infrastructure, but equally to ecosystems as a result of their proliferation: “Quagga mussels affect all the components of the ecosystem – water quality, other wildlife and the room available. They can affect marinas, pipes, the whole water industry and cause a lot of problems.”
Gallardo, along with colleague Dr David Aldridge, refined a model used for predicting the suitability of regions for a particular species to include factors such as population density, land use and the proximity to ports. It is hoped it will lead to a more effective targeting of resources to areas most at risk.
Invasive species are the second biggest threat to biodiversity after habitat loss. Around 12,000 invasive species have already arrived in Europe, where their combined impact on native biodiversity, agriculture, health and the economy costs at least €12 billion a year.
---------------------------
Software described as “pioneering” could change the way in which radiotherapy treatment is administered to cancer patients in the future.
Researchers are looking at the prospect of delivering more personalised courses of treatment by analysing how organs move between radiotherapy sessions to minimise any possible damage to surrounding healthy tissue
Patients have now been recruited for a clinical study to test the computer programs. Up to 1,500 patients with three different types of tumour – prostate cancer, head and neck cancers and cancers affecting the central nervous system – are being recruited to refine the software and determine whether it can indeed help to lessen damage to healthy tissue.
A range of collaborative scientific disciplines are being used as part of a new Cancer Research UK study. Research has shown that organs such as the prostate can move up to two centimetres between sessions, leading to damage which can lead to diarrhoea, for example.
Chief investigator Professor Neil Burnet, a radiotherapy expert from Addenbrooke’s Hospital said: “This [the new software] is particularly crucial for prostate, brain and head and neck cancers, which have important parts of the body nearby that could easily be damaged.
---------------------------
Cambridge scientists have published research which focuses on a new way of tracking the real-time evolution of tumours and how they develop drug resistance by tracking changes in a patient’s blood.
Scientists at the Cancer Research UK Cambridge Institute at the University of Cambridge followed six patients with advanced breast, ovarian and lung cancers and took blood samples, over one to two years. They looked at samples containing a higher concentration of tumour DNA, also known as circulating tumour DNA (ctDNA), and examined changes before and after a course of treatment that were most likely linked to drug resistance.
It is hoped that this new development can lead to research looking at how cancer tumours develop resistance to the most common chemotherapy drugs available at the moment, in addition to a new way of collecting tumour DNA, directly from the tumour, despite being more difficult.
 News / Cambridge MP joins academics in funding cuts criticism8 April 2026
News / Cambridge MP joins academics in funding cuts criticism8 April 2026 News / Rowers fined nearly £4.5k for Lent Bumps misconduct9 April 2026
News / Rowers fined nearly £4.5k for Lent Bumps misconduct9 April 2026 News / Construction begins on controversial Queens’ accommodation6 April 2026
News / Construction begins on controversial Queens’ accommodation6 April 2026 Comment / I’m keeping the em dash7 April 2026
Comment / I’m keeping the em dash7 April 2026 Comment / Reframing the anti-AI ‘performance’9 April 2026
Comment / Reframing the anti-AI ‘performance’9 April 2026








